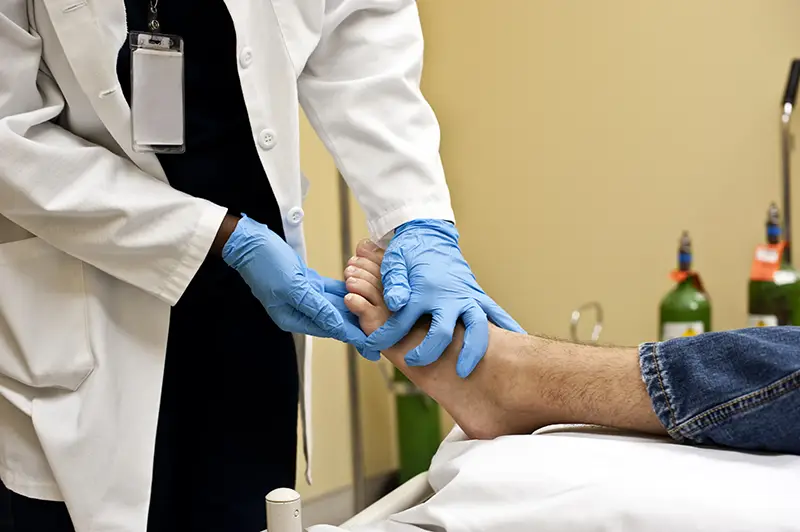
What causes diabetic foot ulcers?
There are several risk factors for developing diabetic foot ulcers:
- Loss of Protective Sensation (LOPS) – high blood glucose can damage nerves leading to neuropathy which may allow injuries to go unnoticed, leading to ulceration.
- Peripheral arterial disease (PAD) – this is sometimes called ‘poor circulation’ and refers to naroowing of the arteries in the legs meaning there is less blood (and oxygen) supply to the muscles.
- Foot deformities – damage to the nerve supply of the foot muscles causes weakening of the muscles and a change in shape of the feet which can create pressure points increasing risk of sores and ulceration
- Previous history – 65% of healed diabetic fool ulcers recur within 3 years 2</sup
Many diabetic foot ulcers are related to trauma caused by wearing uncomfortable shoes, an injury cause when cutting toes nails or to fissures/cracks on the soles of the feet.
Prevention of diabetic foot ulcers
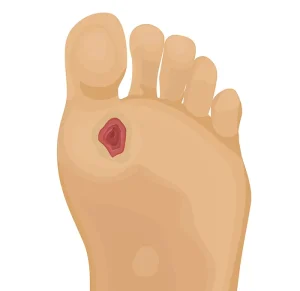
Some of the steps you can take to prevent foot ulceration:
- Glycaemic control – regularly checking and ensuring your blood glucose is within the normal range
- Foot check – check you feet (or get someone else to check your feet) daily for cuts, blisters and wounds. Have regular foot checks with podiatrist, GP or nurse.
- Foot care – wash and dry your feet daily, ensuring you don’t forget to dry between your toes. Use a moisturiser to keep your skin soft.
- Foot wear – ensuring you wear properly fitting footwear is important.
- Avoid walking around barefoot
- Do not wear tight of knee-high socks
- Wear properly fitting footwear – shoes should not be too loose or too
tight, avoid pointed toed shoes - Examine your shoes and socks for damage before putting on to prevent damage to your skin
- an ulcer
- a scratch
- a cut
- a blister
- feel pain
- swelling
- redness
Treatment of diabetic foot ulcers
It’s really important to contact you GP, podiatrist or nurse immediately if you see something wrong – no matter how small the wound.
The important thing to remember is to keep your weight off your foot.
A key factor to close the wound and to avoid complications such as infection and amputation is to react early. It is important that your feet are being taken care of by a team of specialists
For more information on Diabetic Foot Ulcer please visit Save Feet Save Lives